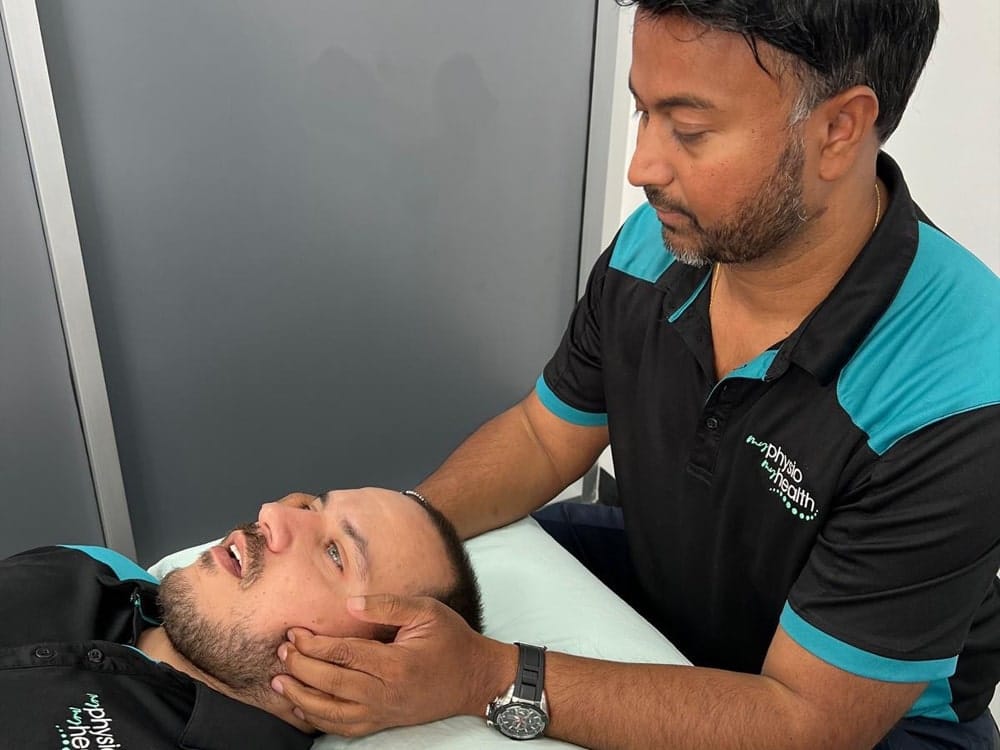
The temporomandibular joint (TMJ) is the joint that connects your jaw to your skull. It allows for the movement required for chewing and talking. Since the TMJ allows for movement both up and down as well as from side to side, it is one of the most complex joints in the body. When this joint is injured or damaged, it can lead to a localized pain disorder called TMJ syndrome or TMJ disorder.
Causes TMJ dysfunction syndrome:
Specialists believe that TMJ dysfunction develops under the influence of many factors. The TMJ belongs to the “target organs” that correspond to aggression factors of different origins. Therefore, they can be either internal or external factors.
Internal factors:
- Inflammatory conditions within the joint are often caused by direct trauma, such as a blow to the chin or jaw, indirect trauma, such as a whiplash injury, heavy chewing, grinding, clenching of the jaw or loss of dental height due to worn down or missing teeth.
- Disc displacement – There is articular disc in the joint; this disc can become displaced in any direction. More commonly, it will be pushed forward during opening and will bunch up. At a certain point in range the disc will reposition or reduce itself causing an audible or palpable click. The jaw will often deviate towards the affected side.
- Arthritis: degenerative wear and tear can occur in the TMJ. It can often be seen on plain x-ray as a flattening of the cartilage head. Other inflammatory arthritic diseases can affect the TMJ, including rheumatoid arthritis, ankylosing spondylitis, infectious arthritis, Reiter syndrome and gout.
- Hyper mobility can result in excessive anterior movement of the jaw and the articular disc. This will result in deviation of the jaw away from the affected side. There are usually some clicking sounds in the TMJ and there may or may not be pain. Hyper mobility may be related to connective tissue disorders such as Down’s syndrome and cerebral palsy
External factors:
- Muscle Spasm can cause significant pain and limitation of movement of the jaw. It often affects one or more muscles, commonly the muscles of mastication, especially masseter, temporalis and the pterygoid muscles. Causes include prolonged dental procedures or anaesthetics where the mouth has been held open for extended periods of time, stress and postural dysfunction.
- Postural Disorders can cause jaw pain. Some of the muscles attach to the jaw originate from the neck; when the head is protracted forward these muscles will pull on the mandible. With prolonged poor posture eventually can cause swelling, pain and gradual degeneration of the disc.
- Fractures of the mandible often occur at the mandibular cartilage. The mechanism of injury can be a blow to the jaw or a fall onto the chin. Treatment can usually begin within a week or two of surgery to begin early mobilisation of the TMJ and to restore function.
There is a range of symptoms linked to TMJ, including:
Pain: One of the most obvious symptoms of a TMJ disorder is pain that is felt when moving the jaw. However, other symptoms that may occur with a TMJ disorder include headaches or migraines, neck ache or backache, and earaches or pain around the ear that spreads to the cheeks.
Sounds: A common but often painless symptom is an unusual popping, clicking, or even grinding noise that can occur while eating, talking, or simply opening the mouth. Buzzing, ringing, or numbness in the ears can occur alongside earaches, and these symptoms can also be associated with TMJ disorders.
Restricted movement: Limited movement that prevents the mouth from being opened fully or the jaw from being moved in certain directions can cause severe discomfort in everyday life.
Physiotherapy Assessment:
As with all areas of physiotherapy, at My Physio My Health we do a thorough examination. It includes assessment of the patient’s posture (position of the jaw, tongue and neck); palpation of the TMJ to assess for swelling, muscle spasm and stiffness or hyper-mobility of one or both TMJ; assessment of range and quality of movement of the jaw and neck, particularly noting any deviation or deflection of the jaw and assessment of the patient’s bite.
Treatment:
Treatment needs to address the issues identified in the assessment. If the patient’s symptoms are acute and inflammatory then their condition is likely to be irritable and one should proceed very gently with the aim of first relieving pain, swelling and muscle spasm. When the pain begins to settle then start to restore jaw movement and alignment. Treatment may include soft tissue releases combined with dry needling to affected muscles and joint mobilisation techniques. It is also important to treat any associated neck pain and headaches. Posture correction is essential and should address head, neck, shoulder and tongue position. The patient should be taught exercises to improve coordination, stability and alignment of the jaw.
My Physio My Health
Trust our team of physiotherapists to help you recover faster and improve your quality of life.

 WISHING EVERYONE A HAPPY NEW YEAR! WE'VE RETURNED TO OUR REGULAR OPENING HOURS
WISHING EVERYONE A HAPPY NEW YEAR! WE'VE RETURNED TO OUR REGULAR OPENING HOURS